Plantar Fasciitis Treatment from a Trusted Tucson Chiropractor
Table of contents
Last Reviewed By: Dr. Christopher Cox, D.C., March 3, 2026
-
- Plantar Fasciitis Treatment in Tucson Non-Surgical Heel Pain Relief That Helps You Stay Active
- Quick Answer: What Helps Plantar Fasciitis Most?
- Understanding Plantar Fasciitis
- Common Signs and Symptoms
- Why Heel Pain Keeps Coming Back
- Red Flags: When to Seek Urgent Care
- How We Assess Plantar Fasciitis in Tucson
- Our Treatment Framework
- What the Science Says (Plain Language)
- Patient Success Story — Plantar Fasciitis Recovery
- Download Our 5-Minute Plantar Fasciitis Morning Reset
- Watch: Why Your Plantar Fasciitis Isn’t Going Away
- Common Questions About Plantar Fasciitis
- Clinical References
- Meet the team
- Book Your Assessment

Plantar Fasciitis Treatment in Tucson Non-Surgical Heel Pain Relief That Helps You Stay Active
If your first steps in the morning feel sharp, stiff, or “knife-like,” or your heel tightens up after standing, walking, or working, you’re not alone. Plantar fasciitis (also referred to as plantar heel pain or plantar fasciopathy) is one of the most common foot complaints we see — and it affects far more than just “active people.” We help runners, healthcare workers, teachers, parents, desk workers, and retirees alike. The real issue is rarely how much you move — it’s how your body is moving, loading, and compensating over time.
The good news is that most cases of plantar fasciitis do not require surgery when approached correctly. With a thoughtful, structured, non-surgical plan that calms irritation, restores mobility, retrains proper movement patterns, and supports the repair of damaged tissue, meaningful and lasting recovery is very achievable. (PubMed)
At Life Aligned Wellness Center in Tucson, we don’t treat plantar fasciitis as “just a foot problem.” In many cases, it isn’t. Sometimes the dysfunction truly starts in the foot, but just as often it begins higher up — in the ankle, calf, knee, hip, pelvis, or even the spine — and travels down the biomechanical chain until the plantar fascia becomes the place where stress finally shows up as pain.That’s why our focus is on unwinding the dysfunctional biomechanical stress that is ultimately manifesting in your heel. We take a true whole-person, full-chain approach: evaluating your posture, gait, foot mechanics, and how your nervous system is adapting to stress. From there, we don’t just “treat” the problem — we help you retrain proper movement, rebuild and repair damaged tissue, and restore more balanced, efficient biomechanics so your body can heal and stay healthy.
We are upfront and honest from the start. Not every case is the right fit for our care, and if we believe you’d be better served elsewhere, we’ll tell you. But when we do take a case, our goal is simple: help you get back to walking, working, and living with confidence — without depending on pain medications, repeated injections, or unnecessary procedures.
Quick Answer: What Helps Plantar Fasciitis Most?
The most effective approach is a phased plan that first reduces tension on irritated tissue, then supports real tissue repair, and only after that rebuilds proper biomechanics and strength.
We avoid aggressive plantar fascia stretching because, while it can feel good temporarily, it often increases stress on already damaged tissue and can make the problem worse over time.
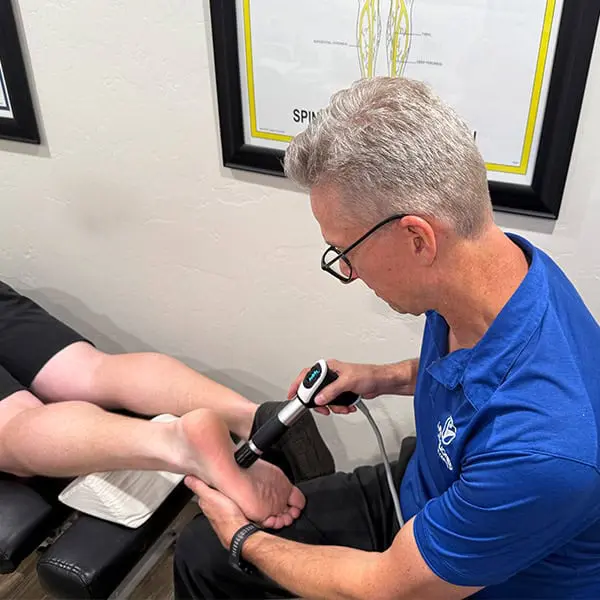
In many cases, we use shockwave therapy to help break up scar tissue and adhesions in the plantar fascia, creating a better environment for healing — especially when paired with individualized rehab. (jospt.org)
Once tissues are healing, we focus on restoring proper movement through the entire biomechanical chain (foot → ankle → leg → pelvis → spine), add appropriate support when needed, and then progressively rebuild strength and tissue capacity.
Important: If you have progressive weakness, major numbness, fever, recent trauma, inability to bear weight, or severe unexplained swelling, seek urgent medical care.
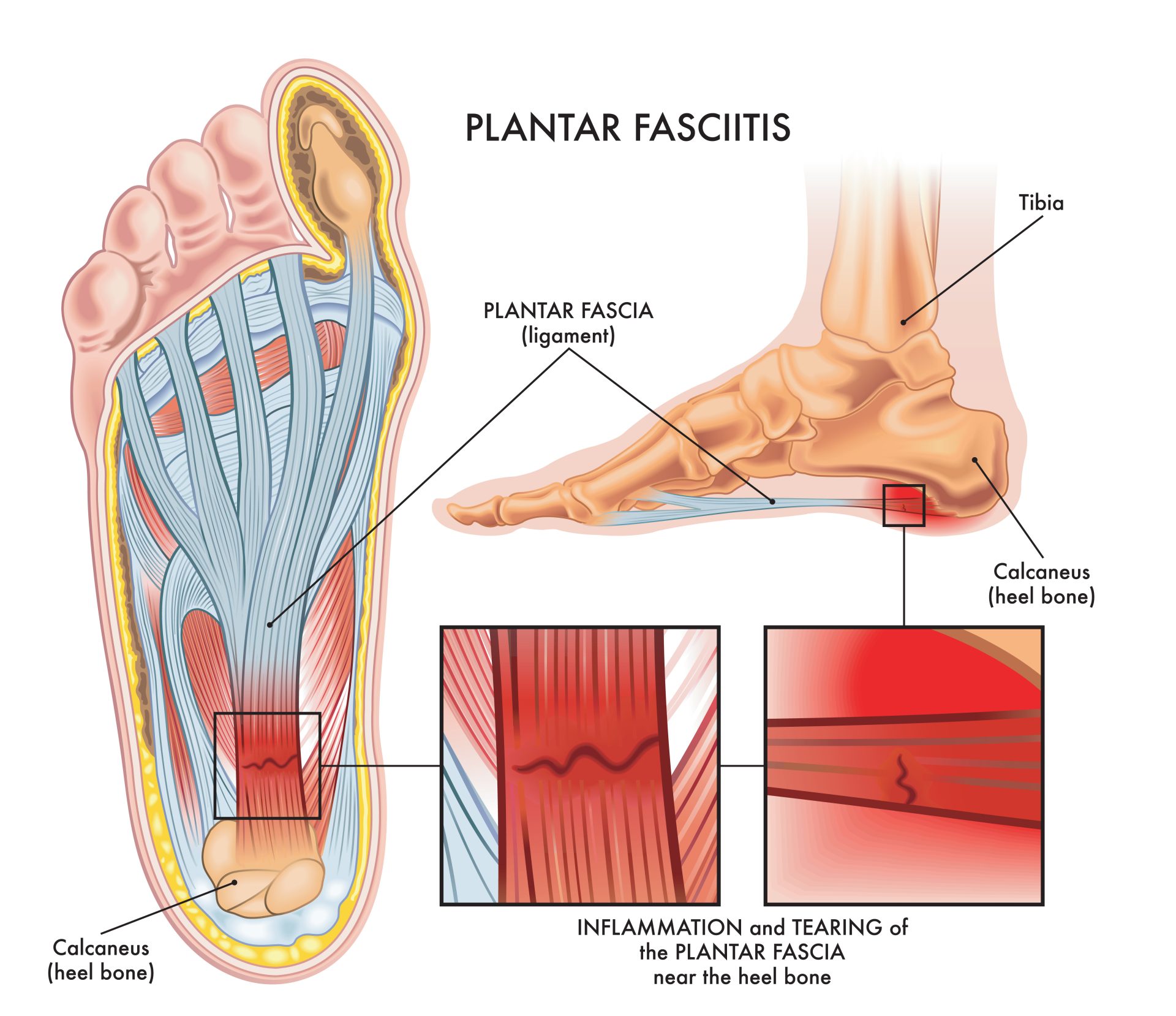
Understanding Plantar Fasciitis
The plantar fascia is a strong, fibrous band of connective tissue that runs along the bottom of your foot. Importantly, it is not the foot’s primary support system — it functions as a secondary suspension system. Your intrinsic foot muscles and ligaments are the primary stabilizers that maintain your arch and control how forces move through your foot with every step.
When this primary system becomes less effective — due to factors like aging, weakness, footwear, altered movement, or repeated asymmetric stress — the plantar fascia is forced to take on more load than it was designed to handle. Over weeks to months, that chronic excess tension can exceed the tissue’s ability to adapt and repair, and plantar fasciitis develops.
Why first steps hurt most
A classic pattern is sharp pain with your first steps in the morning or after sitting. At rest, the irritated tissue stiffens and tightens. When you stand, that sudden load on a compromised plantar fascia produces the familiar “first-step pain.” Symptoms may ease as you move, then return later in the day as the tissue fatigues with standing, stairs, errands, or activity.
Is it always a heel spur?
No. Heel spurs are commonly seen on imaging, but they are typically a long-term bony response to chronic abnormal tension on the plantar fascia — not the original cause of pain. Many people have heel spurs with no symptoms, while others have significant pain without one. What matters most are your symptoms, movement patterns, and physical exam findings — not imaging alone.
Common Signs and Symptoms:
Persistent Pain
Sharp or deep aching pain along the bottom or inner side of the heel
Radiating Pain
Pain with the very first steps in the morning or after sitting for a while
Limited Mobility
Increased pain after prolonged standing, walking, or shifts on your feet
Pain with Activity
Tenderness when pressing near the inside of the heel where the plantar fascia attaches
Non-Drug Relief
Symptoms often feel better once you “warm up,” then flare again later in the day as the tissue fatigues
People with plantar fasciitis typically notice a predictable pattern of symptoms, especially as tissue irritation and abnormal tension build over time.
This pattern reflects irritated tissue being repeatedly overloaded — which is why our focus is not just on calming symptoms, but on reducing tension, repairing tissue, and correcting the underlying biomechanics that are driving the problem.
Why Heel Pain Keeps Coming Back
For many people, recurring plantar heel pain is fundamentally a load and biomechanics problem — not just a “foot” problem. The plantar fascia usually isn’t failing in isolation; it’s responding to how forces are moving through your body over time. Common contributors include:
- Load spikes
Sudden increases in steps, new workouts, longer work shifts, or a rapid return to activity can overload irritated tissue before it has fully healed. - Mobility limits
Restricted ankle dorsiflexion or excessive calf stiffness can shift more tension onto the plantar fascia, increasing stress with every step. - Capacity gap
Even when pain improves, the foot and calf tissues may not yet have enough strength or resilience to tolerate your current daily or athletic demands. - Footwear mismatch
Shoes that don’t fit your foot, your job, or your activity can alter how load travels through your foot and prolong irritation. - Whole-chain mechanics
How your hips, knees, pelvis, and trunk move and stabilize directly influences repetitive stress on your foot. If there are imbalances higher up the chain, the plantar fascia often becomes the weak link.
This is why lasting recovery requires more than symptom relief — it requires reducing abnormal tension, repairing tissue, and restoring balanced movement throughout the entire biomechanical system.
Red Flags: When to Seek Urgent Care
While most cases of plantar heel pain are mechanical and respond well to conservative care, certain symptoms suggest something more serious that requires prompt medical evaluation. Seek urgent care or contact your physician right away if you experience:
- Sudden trauma with inability to bear weight on the foot
- Progressive or worsening weakness in the foot or leg
- Persistent numbness, tingling, or significant neurologic symptoms
- Fever, redness, warmth, or unexplained swelling around the heel or foot
- Night pain that is severe or accompanied by systemic illness symptoms
This information is educational and does not replace emergency medical care.

How We Assess Plantar Fasciitis in Tucson
A successful recovery begins with a precise diagnosis and a clear understanding of how irritable your tissues currently are — and why they became that way in the first place. Our evaluation is designed to identify the true root cause of your heel pain, not just the location of your symptoms.
Your assessment typically includes:
- Detailed symptom history — what provokes your pain, what relieves it, and how it behaves throughout the day
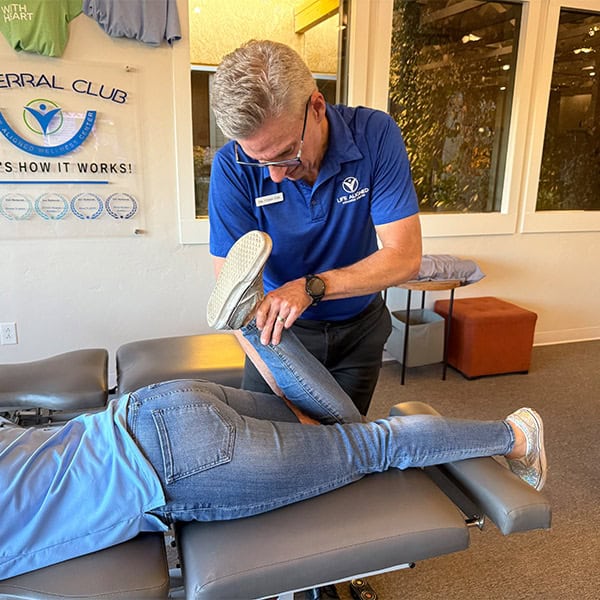
- Hands-on exam of the foot and ankle, including palpation and movement testing of key joints and soft tissues
- Calf strength/endurance and ankle mobility testing to determine whether a capacity or mobility gap is contributing to your symptoms
- Gait and loading analysis to see how forces are moving through your body when you walk or stand
- 3D functional movement analysis, balance assessment, and foot-strike measurement to understand how you actually move in real time
- Whole-body biomechanical evaluation (foot, ankle, leg, pelvis, and spine) to see where abnormal stress is originating
- Nervous system assessment to determine whether your “master movement control system” is allowing you to move in a normal, efficient biomechanical way
- Differential screening to distinguish plantar fascia involvement from other possible sources of pain (nerve irritation, Achilles issues, fat pad irritation, stress reactions, etc.)
- Imaging referral only when clinically necessary, not as a routine first step
This approach allows us to determine where the root of the problem truly lies, how long this has likely been a functional issue (not just symptomatic), and to give you a realistic, transparent timeframe for recovery.
At Life Aligned Wellness Center, our patient journey starts with a consult-first approach so we can quickly understand your situation and determine the best next steps. For those in significant pain, we also offer direct phone booking to prioritize urgent needs and get you evaluated without unnecessary delays.
Our Treatment Framework
Phase-Based, Personalized, and Non-Surgical
This timeline provides a general framework for what recovery often looks like — because most people want to know what to expect. However, it’s important to understand that no two patients are the same. Every person is assessed individually, and your progression through these phases may be faster, slower, or look slightly different depending on your biomechanics, irritability level, activity demands, and how long this has been a functional problem in your body (not just how long it has hurt).
We also individualize when and howwe use different therapies. In many cases, we begin shockwave early, rehab starts shortly after based on your tolerance, and chiropractic care to address foundational biomechanical and nervous system dysfunction begins right away when indicated.

Phase 1 (Weeks 0–2): Calm Irritation
The goal is to reduce tension on irritated tissue and create a true healing environment — not to shut you down.
- Modify step volume and high-irritation tasks (not complete rest)
- Footwear and standing strategy updates to reduce unnecessary load
- Shockwave therapy is often started in this phase to help break up scar tissue/adhesions and stimulate tissue repair
- Early, pain-modulated movement and rehab begins as soon as your tolerance allows
- Chiropractic care starts right away when indicated to address foundational biomechanical and nervous system dysfunction
- We do not rely on temporary supports or taping
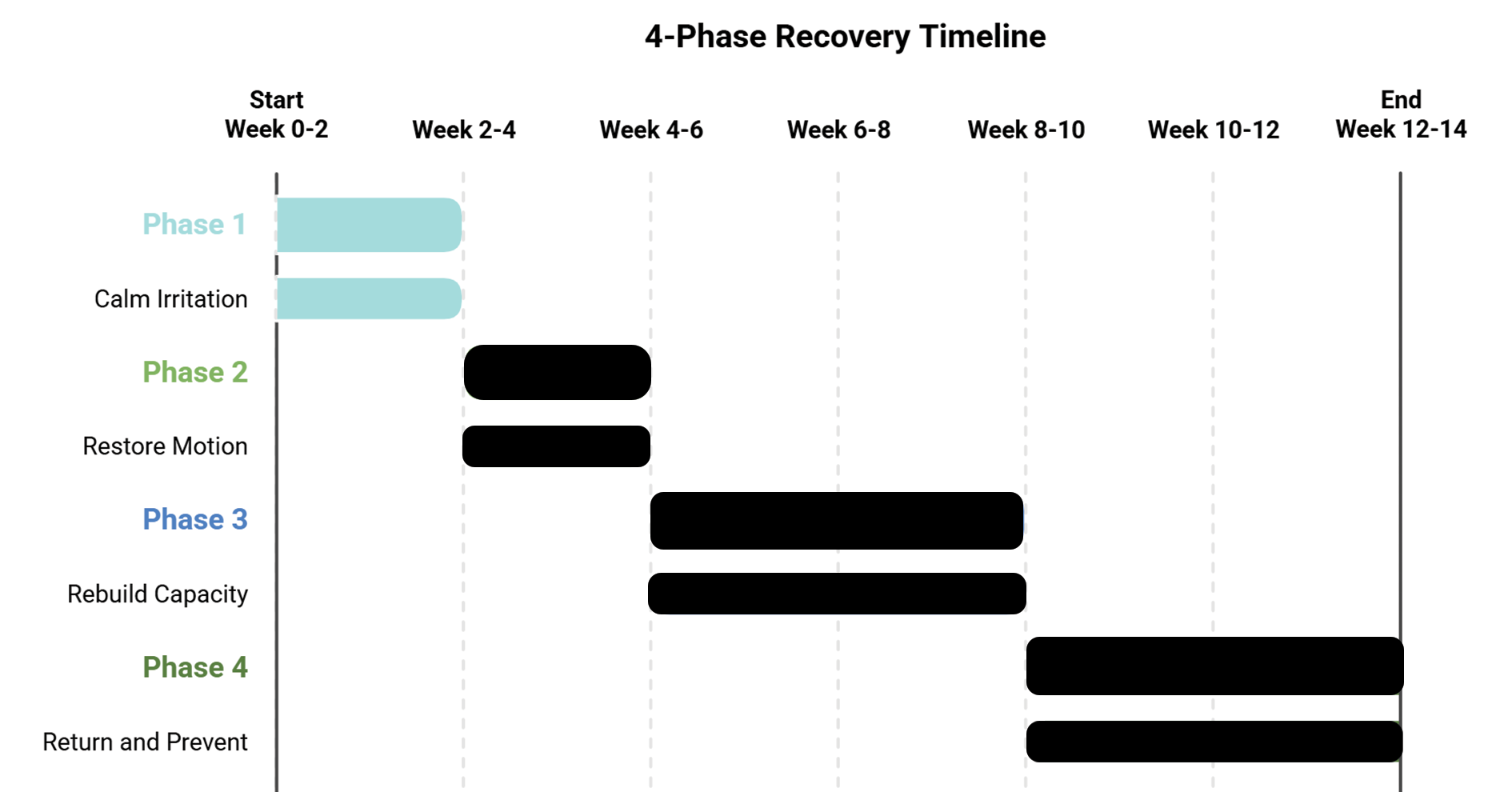
Phase 2 (Weeks 2–4): Restore Motion
Once irritation is settling, we focus on normal movement.
- Progressive foot and ankle mobility work
- Calf and Achilles mobility strategies as indicated
- Continued shockwave when appropriate
- Manual therapy and soft-tissue techniques when they will meaningfully improve tissue quality and movement
- Ongoing rehab progression based on your response

Phase 3 (Weeks 4–8): Rebuild Capacity
Now the emphasis is on repairing and strengthening what has been overloaded.
- Progressive calf and plantar fascia loading
- Targeted foot intrinsic strengthening to restore the foot’s primary support system
- Controlled return to walking and activity matched to your tolerance
- Continued movement and chiropractic care as needed to maintain proper biomechanics
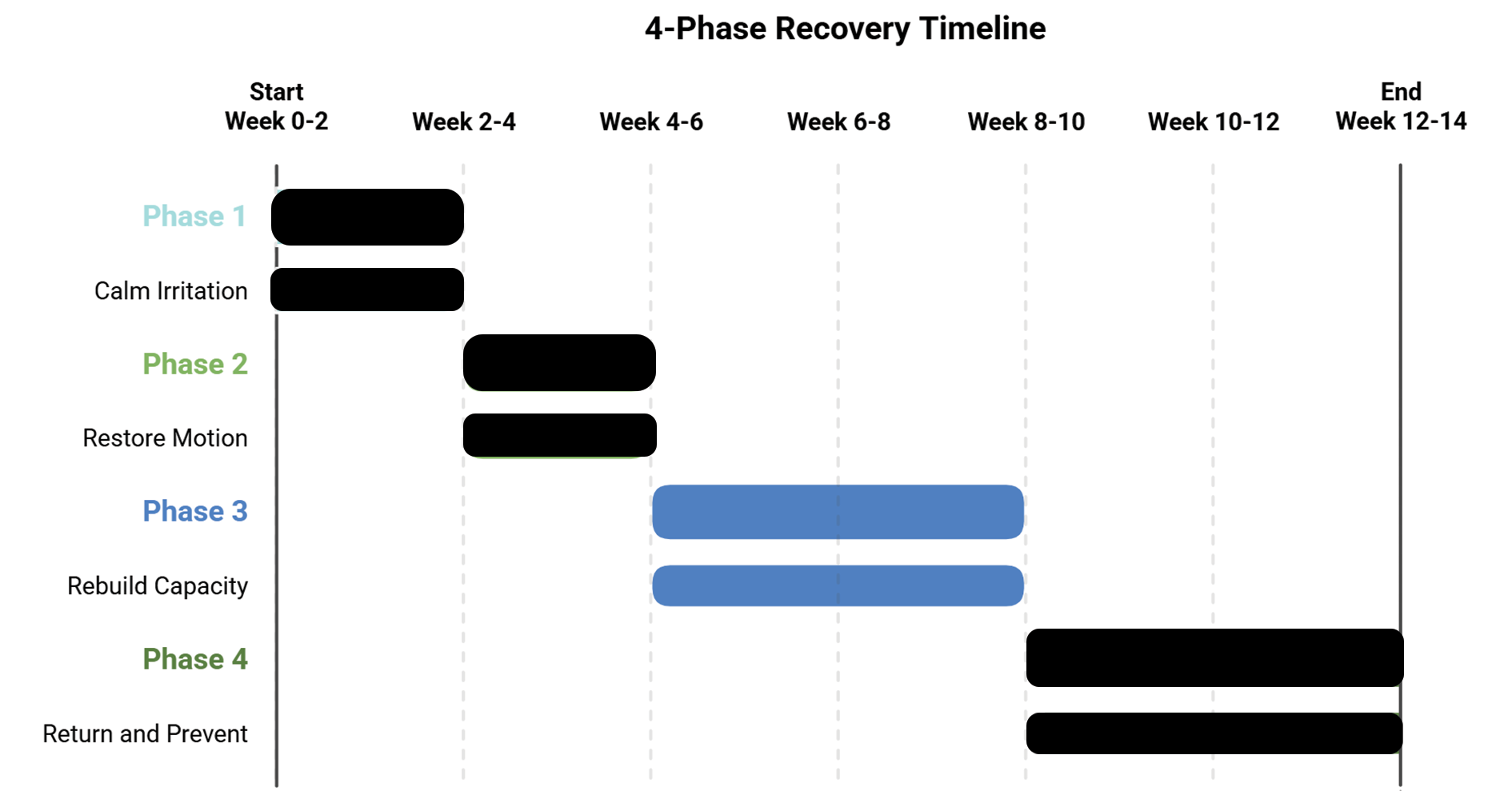
Phase 4 (Weeks 8+): Return and Prevent
This phase is about durability — not just symptom relief.
- Gradual return-to-work and return-to-fitness plan
- Clear flare-up management rules so small setbacks don’t become big ones
- Long-term habits for recurrence prevention (movement, strength, and footwear strategies)
- Orthotics are re-evaluated around 8 weeks — only after we’ve helped your body function as close to normal as possible. We do not want to support or “lock in” an imbalanced state.

What the Science Says (Plain Language)
Recent guidance and evidence support a multimodal, conservative-first strategy:
- The 2023 heel pain clinical practice guideline supports interventions such as manual therapy, stretching, taping, and progressive exercise/loading strategies tailored to the individual. (jospt.org)
- A best-practice guide in sports medicine recommends core care including individualized education, stretching, and taping, with escalation based on response. (British Journal of Sports Medicine)
- Meta-analytic evidence suggests shockwave can improve pain and function in chronic plantar fasciitis for many patients, though protocols and comparative outcomes vary. (PubMed)
Broad clinical references continue to position conservative treatment as first-line before surgical escalation in most cases. (BMJ Best Practice)
Patient Success Story — Plantar Fasciitis Recovery
From painful every step to moving with confidence again
After nearly two years of stubborn heel pain in both feet, this patient had to give up daily walks and many of the activities they loved. Shoes, inserts, stretching, ice, and over-the-counter pain relievers hadn’t helped—and with a history of type 1 diabetes, healing felt slow and frustrating.
A different approach
Rather than treating only the feet, care focused on the body as a connected system and included:
- Specific chiropractic adjustments to improve nerve and joint function
- Radial shockwave therapy to stimulate healing in the plantar fascia
- Gentle soft-tissue work
- Customized exercises for the feet, ankles, and gait
- Ongoing progress checks to guide treatment
Real results — in about 4 months
With consistent care, the patient experienced:
- 70–75% overall improvement in plantar fasciitis
- Markedly better pain and function in the more painful foot
- Easier, smoother walking with less hesitation
- Noticeably less back and hip soreness along the way
- Better tolerance for daily movement and standing
- Renewed confidence that an active lifestyle was possible again

One area of the foot needed a slower, gentler pace of shockwave along the way—but the overall trajectory remained strongly positive.
Quality of life that mattered
This wasn’t just about “less pain.” The patient regained freedom to move, felt more balanced in their body, and began getting back to the activities they enjoy.
“Treating my whole body—not just my feet—made all the difference.
Download Our 5-Minute Plantar Fasciitis Morning Reset
Give your feet a gentler start to the day. This downloadable guide includes a simple 5-minute morning reset, flare-day tips, starter exercises, common aggravators to avoid, and important red flags to watch for. It is a practical, easy-to-follow resource for anyone dealing with plantar fasciitis and looking for clear next steps at home.

Plantar Fasciitis in Tucson: Why Heel Pain Persists and What Helps
FAQs
Clinical References
Heel Pain – Plantar Fasciitis: Revision 2023 (JOSPT CPG). (jospt.org)
Management of Plantar Heel Pain: Best Practice Guide (BJSM, 2021). (British Journal of Sports Medicine)
ESWT meta-analysis evidence for chronic plantar fasciitis. (PubMed)
BMJ Best Practice: plantar fasciitis diagnosis/management overview. (BMJ Best Practice)
Life Aligned Wellness service/tone references. (Life Aligned Wellness)
Meet The Team





What Our Patients Are Saying
Making Great Healthcare Affordable
At Life Aligned Wellness Center in Tucson, we recognize that everyone’s health and goals are unique. After discussing your objectives, we’ll assess the issue and provide tailored recommendations to help you achieve them. As an out-of-network provider, we offer customized care plans and flexible payment options, including financing. Our patients consistently find our care to be one of the best investments in their well-being.
schedule a consultation now
