
Low Back Pain Treatment in Tucson: Evidence-Based, Non-Surgical Care
Table of Contents
Last Reviewed By: Dr. Christopher Cox, D.C., April 24th, 2026
-
- Quick Answer: What You Need to Know About Low Back Pain
- What Is Low Back Pain, Really?
- How Low Back Pain Shows Up in Daily Life
- Warning Signs That Require Urgent Medical Attention
- How We Assess Your Case at Life Aligned
- Your Personalized Treatment Plan: A Phased Approach to Recovery
- What the Research Says: An Evidence Snapshot
- Patient Case Study: From Morning Stiffness to Full Activity
- Free Download: Your Low Back Pain Recovery Guide
- Frequently Asked Questions
- References
- Meet Your Doctor
- What Our Patients Are Saying
- Ready to Start Feeling Better in Tucson?

Quick Answer: What You Need to Know About Low Back Pain
Low back pain is one of the most common reasons people miss work, avoid activities they love, and end up cycling through treatments that never quite fix the problem. It occurs when structures in the lumbar spine, including the vertebrae, discs, joints, nerves, and surrounding muscles, are irritated, compressed, or functioning poorly. The most common causes include muscle strain, disc irritation, sacroiliac joint dysfunction, and poor spinal mechanics from prolonged sitting or repetitive movement. For most people, conservative care like chiropractic treatment and targeted rehabilitation is the appropriate first step. Seek urgent care if your pain follows a traumatic injury, is accompanied by numbness or weakness in both legs, or includes loss of bladder or bowel control.

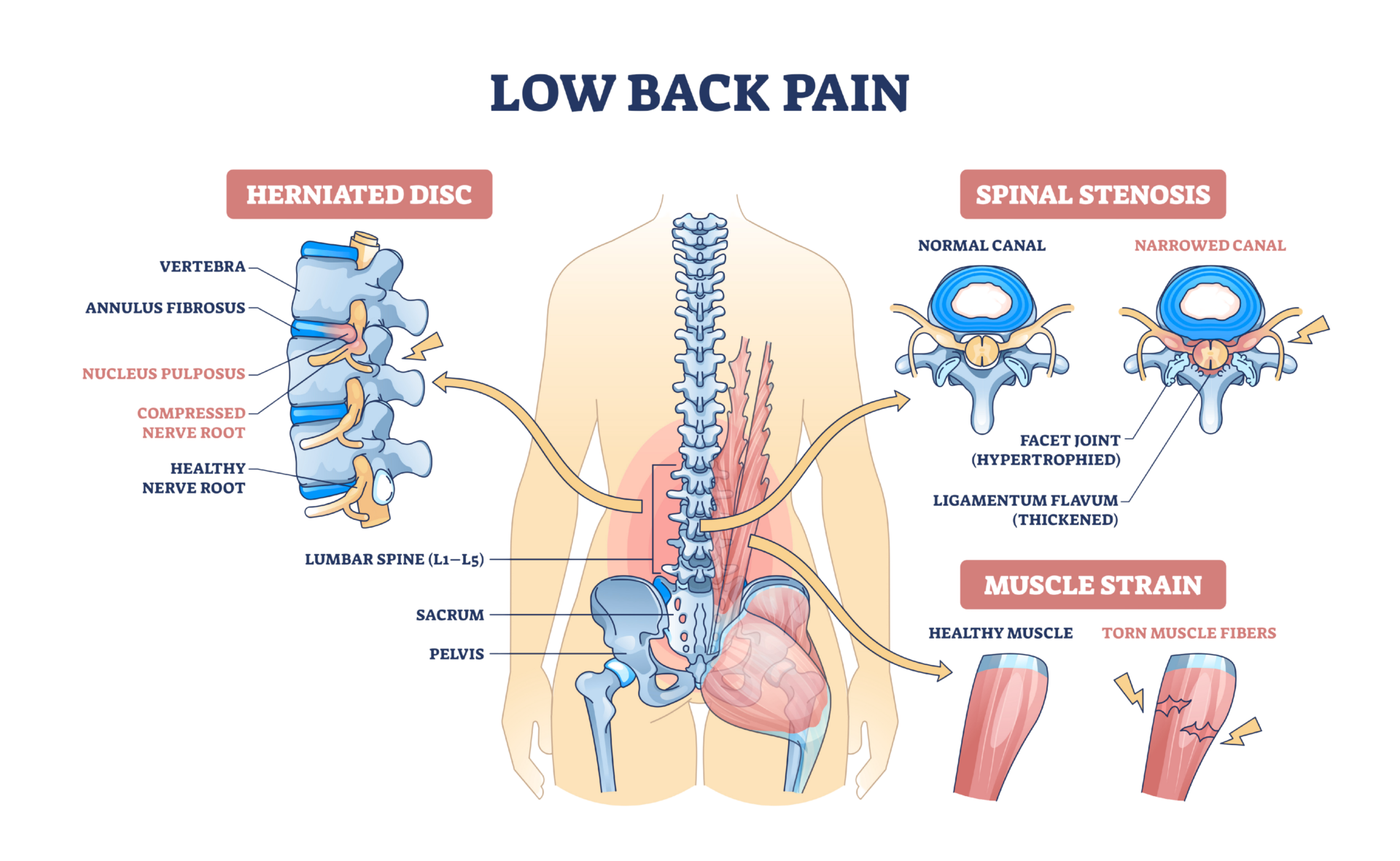
What Is Low Back Pain, Really?
Low back pain is not a single condition. It is a symptom with many possible sources, and that distinction matters enormously when it comes to finding lasting relief.
The lumbar spine, the five vertebrae that make up your lower back, carries the majority of your body weight with every step you take, every hour you sit, and every load you lift. When any part of that system, whether a disc, a joint, a nerve, or a supporting muscle, is not moving or functioning as it should, pain is often the result.
Low back pain is generally described as either acute or persistent. Acute low back pain typically comes on suddenly, often after a specific movement or event, and tends to resolve within a few weeks with appropriate care. Persistent low back pain, sometimes called chronic low back pain, lasts longer than three months and often involves a combination of mechanical dysfunction, deconditioned tissues, and movement habits that continue to load the spine in unhelpful ways.
Two common myths are worth addressing directly. The first is that back pain always means something is seriously wrong or damaged beyond repair. The reality is that many people experience significant pain from issues that are highly responsive to conservative care. The second myth is that rest is the best medicine. Current evidence consistently shows that remaining gently active, guided by qualified care, leads to better outcomes than prolonged bed rest.
How Low Back Pain Shows Up in Daily Life
Low back pain is not just a sensation in your spine. For most people, it reshapes how they move, sleep, work, and live.
The most commonly reported symptoms include:
-
- A dull, aching sensation across the lower back that worsens after sitting for long periods
- Sharp or stabbing pain with certain movements like bending forward, twisting, or standing up from a chair
- Stiffness and restricted range of motion in the morning that gradually loosens as the day goes on
- Pain that radiates into the buttocks, hips, or down one or both legs
- A sense of instability or weakness in the lower back, particularly under load
- Muscle spasms that can make even small movements feel unpredictable and uncomfortable
Certain patterns tend to aggravate symptoms. Prolonged sitting is one of the most consistent aggravating factors, which is why so many people find that driving or desk work triggers a flare. Bending forward repeatedly, standing on hard surfaces for extended periods, and high-impact activities can all intensify pain depending on its source. Many people find relief with movement, gentle walking, or lying in a supported position with the knees bent.
The functional impacts of low back pain extend well beyond the physical. Sleep is frequently disrupted, either from difficulty finding a comfortable position or from pain that wakes you through the night. Work performance suffers, especially in jobs that require sitting, lifting, or standing. Exercise, recreation, and even simple daily tasks like putting on shoes or loading the dishwasher become challenging. For many patients, this steady erosion of normal activity compounds the problem, as reduced movement weakens the very structures that support the spine.

Warning Signs That Require Urgent Medical Attention
Chiropractic care is appropriate for the vast majority of low back pain presentations. There are, however, specific warning signs that require prompt medical evaluation rather than conservative treatment. If you experience any of the following, please contact a physician or emergency services before booking a chiropractic appointment.
Seek urgent care if you have:
-
- Low back pain that follows a significant fall, vehicle accident, or direct impact to the spine
- Loss of bladder or bowel control, or new difficulty controlling urination or defecation
- Progressive weakness, numbness, or tingling in both legs simultaneously
- Low back pain accompanied by fever, unexplained weight loss, or night sweats
- Pain that is constant, severe, and does not change with any position or movement
- A history of cancer, osteoporosis, or long-term steroid use combined with new or worsening back pain
- Saddle anaesthesia, meaning numbness in the inner thighs, groin, or perineal region
These presentations may indicate serious underlying conditions, including cauda equina syndrome, spinal fracture, infection, or systemic illness, that require imaging and medical management before or alongside any other care. At Life Aligned, our position is straightforward: if we cannot help you, we will tell you who can.

How We Assess Your Case at Life Aligned
Effective treatment begins with an accurate understanding of what is driving your pain. At Life Aligned Wellness Center, Dr. Cox takes the time to assess your case thoroughly before recommending any course of care.
Health History and Symptom Interview
Your first visit begins with a detailed health history. We want to understand not just where your pain is located, but how long you have had it, what makes it better or worse, how it affects your daily life, and what you have already tried. This context shapes everything that follows.
Physical and Functional Examination
Dr. Cox performs a thorough physical examination that includes postural assessment, range of motion testing, orthopaedic and neurological screening tests, and palpation of the lumbar spine and pelvis. Functional testing may be included to assess how your spine performs under real movement demands, not just in a static position.
Differential Diagnosis
Not every case of low back pain has the same source. The assessment process is designed to identify the most likely pain generators, whether that is a disc, a joint, a muscle, a nerve, or a combination of structures, and to rule out presentations that require referral before treatment begins.
Imaging: When It Is and Is Not Needed
Imaging is not always necessary at the outset of care. Current clinical guidelines suggest that routine X-rays and MRI scans for non-specific low back pain without red flags are unlikely to change early management and are not always correlated with a patient’s level of pain or function. When imaging is clinically indicated, based on specific examination findings, a history of trauma, or a failure to respond to initial care, Dr. Cox will refer you for appropriate imaging and factor those results into your plan.

Your Personalized Treatment Plan: A Phased Approach to Recovery
Low back pain rarely resolves with a single intervention. Lasting results come from a structured, phased approach that meets you where you are and moves you progressively toward full function. Here is how care typically unfolds at Life Aligned Wellness Center.
Phase 1: Calm Irritation and Restore Comfort
The first goal is to reduce pain and inflammation enough that your body can begin the healing process. During this phase, Dr. Cox uses specific chiropractic adjustments to address restricted or dysfunctional spinal segments, reduce pressure on irritated nerve tissue, and restore more normal movement to the lumbar spine and pelvis. Soft tissue work may be incorporated where muscle guarding or myofascial restrictions are contributing to your symptoms. The frequency of visits during this phase is typically higher, as the nervous system and surrounding tissues need consistent input to begin shifting out of the pain cycle.

Phase 2: Restore Motion and Neuromuscular Control
As pain begins to settle, the focus shifts to restoring full range of motion and improving the quality of how your spine moves. Targeted mobility work, joint mobilization, and the early introduction of therapeutic exercises help your body relearn efficient movement patterns. This is also when we begin addressing the movement habits and postural tendencies that may have contributed to your pain in the first place.

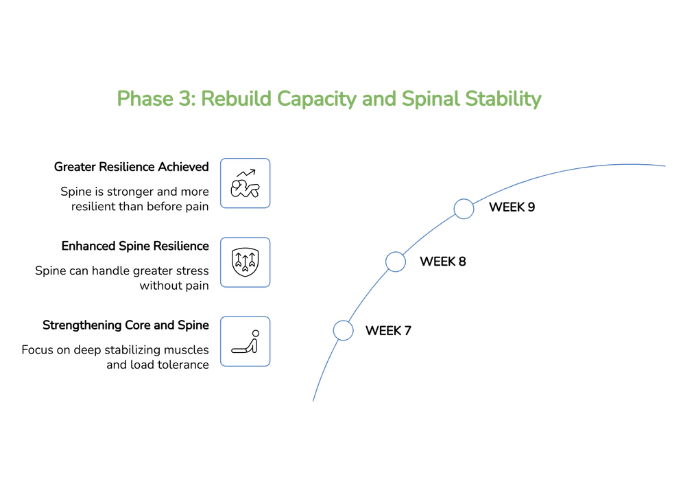
Phase 3: Rebuild Capacity and Spinal Stability
This phase is where durable recovery is built. Progressive rehabilitative exercises are used to strengthen the deep stabilizing muscles of the lumbar spine and core, improve load tolerance, and close the capacity gap that left your spine vulnerable in the first place. The goal is not just to feel better, but to be genuinely more resilient than before your pain began.
Phase 4: Return to Activity and Long-Term Function
As you approach full recovery, care transitions to supporting your return to all the activities that matter to you, whether that is sport, work demands, travel, or simply getting through a day without thinking about your back. Maintenance care recommendations and self-management strategies are provided so you have the tools to protect what you have gained long after your active care has ended.

Adjunct Technologies (Applied Based on Clinical Indication)
For appropriate cases, the following technologies may be incorporated into your care plan:
Shockwave Therapy: Acoustic wave therapy that stimulates cellular repair, improves blood flow, and reduces chronic pain in tendons and soft tissue structures. Particularly useful in persistent cases where tissue healing has stalled.
Spinal Decompression: Motorized traction therapy designed to gently reduce intradiscal pressure and create a negative pressure environment within the disc, which may support retraction of herniated disc material and improved nutrient exchange. Best suited for disc-related low back pain and sciatica.
Not every modality is right for every patient. The decision to incorporate any adjunct technology is based on your specific clinical findings, your response to care, and whether the evidence supports its use for your presentation. Dr. Cox will explain the rationale for any recommendation clearly before it becomes part of your plan.

What Recovery Can Look Like: A Patient Case Study
The following is a de-identified case drawn from the types of presentations seen regularly at Life Aligned Wellness Center. It is provided for educational purposes.
Patient Profile: A 47-year-old office administrator presented with a nine-month history of persistent lower back pain and intermittent pain radiating into the right buttock and posterior thigh. She described her pain as a constant dull ache that spiked to sharp with prolonged sitting and first thing in the morning. She had tried over-the-counter anti-inflammatory medication and rest with only temporary and partial relief.
Baseline Limitations: She was unable to sit comfortably for more than 20 to 25 minutes, had stopped her regular evening walks, and reported that disrupted sleep was affecting her energy and mood at work.
Assessment Findings: Examination revealed restricted lumbar segmental mobility at L4 and L5, mild right-sided sacroiliac joint dysfunction, reduced hip extension, and a positive straight leg raise at 45 degrees on the right. Neurological screening was intact. No red flags were identified. Imaging was not indicated at the initial visit.
Care Plan: Dr. Cox recommended a 10-week active care plan consisting of three visits per week for four weeks, followed by two visits per week for three weeks, and then once per week for three weeks with reassessment at the midpoint.
Interventions: Lumbar and sacroiliac chiropractic adjustments, soft tissue therapy to the right hip and gluteal musculature, progressive home exercise programme targeting hip mobility and core stabilization, and four sessions of spinal decompression therapy during weeks three through five.
Milestones: By week two, morning stiffness had reduced by approximately half and she was sleeping through the night on four of seven nights. By week four, she had returned to short evening walks of 15 to 20 minutes and had increased her comfortable sitting tolerance to 45 minutes. By week eight, her pain had reduced substantially, she had resumed her full walking routine, and she reported feeling confident managing her symptoms with her home programme.
Outcome: Oswestry Disability Index scores at discharge reflected a shift from moderate disability to minimal disability. She was discharged to a once-monthly maintenance care schedule and a self-directed exercise programme.
Maintenance: Plan Monthly spinal maintenance visits and continuation of her home stabilization exercises with a 12-week reassessment scheduled.

What the Research Says: An Evidence Snapshot
At Life Aligned, we believe patients deserve to know what the evidence actually supports. Below is a plain-language summary of the key research relevant to chiropractic care for low back pain.
Spinal Manipulation for Low Back Pain: A 2017 systematic review and meta-analysis published in JAMA found that spinal manipulative therapy produced statistically significant reductions in pain intensity and functional disability in patients with acute low back pain compared to sham treatment or other active therapies. This evidence applies most strongly to adults with non-specific low back pain. It does not speak to all sub-types of back pain, and individual responses vary.
Chiropractic Care Versus Usual Medical Care: A study published in Spine compared chiropractic care to standard medical care for low back pain and found that patients in the chiropractic group reported greater satisfaction and similar or superior pain and function outcomes at comparable cost. Limitation: this comparison reflects general medical care and may not apply to all specialist physician management.
Clinical Practice Guidelines: The American College of Physicians updated its low back pain guidelines in 2017 to recommend non-pharmacological treatments, including spinal manipulation, heat therapy, massage, and exercise, as first-line care for both acute and chronic low back pain. This guideline shift represents a significant move away from immediate reliance on medication and toward conservative, active care approaches.
Spinal Decompression for Disc-Related Low Back Pain: Studies evaluating motorized lumbar traction and decompression therapy have shown meaningful reductions in pain and improved function in patients with herniated discs and degenerative disc disease. Evidence quality is moderate; outcomes are most predictable in patients who present with disc-confirmed radiculopathy.
Exercise and Rehabilitation for Chronic Low Back Pain: Multiple high-quality systematic reviews, including those published in The Cochrane Database, support exercise therapy as one of the most effective interventions for chronic low back pain. Core stabilization, general strengthening, and graded activity all show consistent benefit. Exercise is not a one-size-fits-all prescription, and supervision by a qualified provider improves adherence and outcomes.
Download our “Understanding Your Lower Back Pain” Guide
Give your lower back the clarity it deserves. This downloadable guide includes an overview of common causes of lower back pain, a structured four-phase approach to lasting relief, research-backed treatment options, red flags to watch for, and simple next steps toward care. It is a practical, easy-to-follow resource for anyone dealing with lower back pain and looking for honest answers and a clear path forward.

Frequently Asked Questions About Low Back Pain
Clinical References
Paige, N.M., et al. (2017). Association of Spinal Manipulative Therapy with Clinical Benefit and Harm for Acute Low Back Pain. JAMA, 317(14), 1451 to 1460.
Qaseem, A., et al. (2017). Noninvasive Treatments for Acute, Subacute, and Chronic Low Back Pain: A Clinical Practice Guideline from the American College of Physicians. Annals of Internal Medicine, 166(7), 514 to 530.
van Tulder, M., et al. (2006). Exercise Therapy for Low Back Pain: A Cochrane Systematic Review. Spine, 31(2), 154 to 162.
Slade, S.C. and Keating, J.L. (2006). Trunk-Strengthening Exercises for Chronic Low Back Pain: A Systematic Review. Journal of Manipulative and Physiological Therapeutics, 29(2), 163 to 173.
Hayden, J.A., et al. (2005). Systematic Review: Strategies for Using Exercise Therapy to Improve Outcomes in Chronic Low Back Pain. Annals of Internal Medicine, 142(9), 776 to 785.
What Our Patients Are Saying
Meet The Team





Ready to Start Feeling Better in Tucson?
If you have been managing low back pain on your own, you know how exhausting that cycle becomes. The pain flares, you rest, things settle slightly, and then it comes back. Breaking that cycle requires understanding what is actually driving your symptoms and building a plan that addresses it properly.
At Life Aligned Wellness Center, your first visit is a conversation as much as it is an examination. Dr. Cox takes the time to understand your history, your goals, and your life before recommending any course of care. There are no pressure tactics and no one-size-fits-all protocols. If chiropractic care is appropriate for your case, we will tell you exactly why and show you what the path forward looks like. If it is not the right fit, we will tell you that too and make sure you are pointed in the right direction.
Patients are seen at 7290 E Broadway Blvd Ste. 124, Tucson, AZ 85710. Appointments can be booked online 24 hours a day, seven days a week, or by calling (520) 731-9595.
Book Your Consultation
